Welcome!
Open Door’s 24-month Advanced Practice Clinician (APC) Residency program was established in 2016. The program provides intensive training in the clinical complexity of family practice both in the safety-net setting and in a high-performance, patient-centered medical home (PCMH) model of primary care.
Our program is specifically intended for newly graduated family nurse practitioners (FNP) and physician assistants (PA) who are committed to practicing as primary care providers (PCP) in the challenging setting of community health centers and other safety-net settings.
We’re training the residents in Open Door’s model of high-performance health care: advanced access scheduling, planned care, the chronic care model, integrated behavioral health and primary care, team-based, with expert use of health information technology and the electronic health record (EPIC).
The residency year begins with intensive orientation to Open Door Community Health Centers, the neighborhoods in which the training sites are located, and the health problems of the target population, and includes walking tours of neighborhoods, tours of Open Door sites statewide, meetings with community leaders, technical training on the electronic health record, and orientation by our chief medical officer to the responsibilities and privileges of medical staff participation at Open Door.


Statement of purpose:
We aim to create a unique and comprehensive primary care postgraduate training year for Advanced Practice Clinicians interested in working in rural, low resource areas, and equip them with the necessary skills to provide compassionate, evidence-based care to an underserved, medically complex patient population such as that of Humboldt County.
Our Commitment to Diversity, Equity, and Inclusion:
We are dedicated to recruiting and retaining a diverse group of faculty and residents committed to maintaining a high standard of excellence and cultivating an environment of ongoing learning and growth; building a workforce that is inclusive and representative of the wonderful communities we serve.
About Us
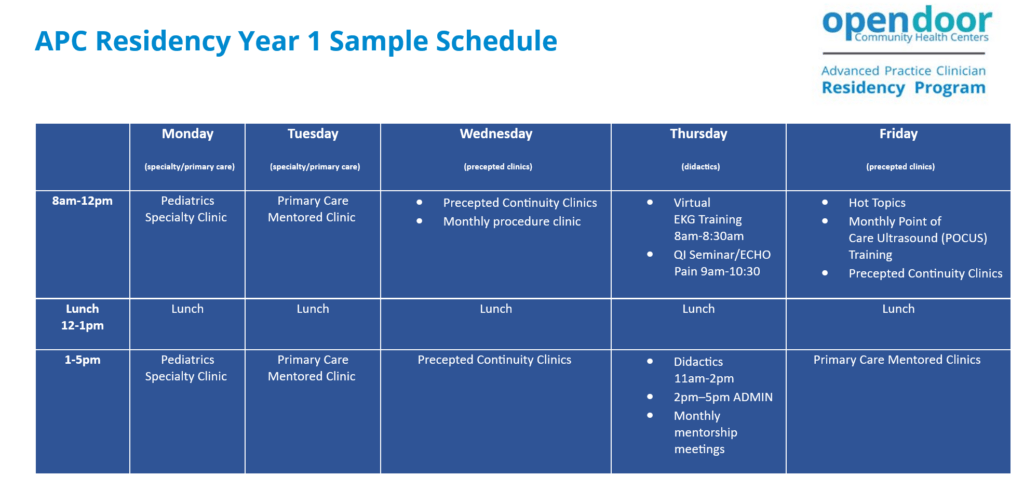
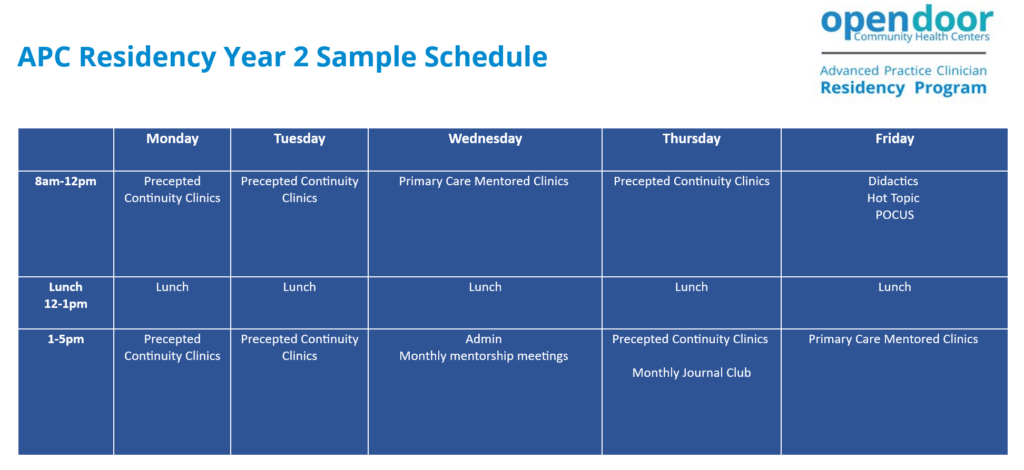
Program Structure

What Makes Us Unique?

Humboldt County Attractions

Qualifications

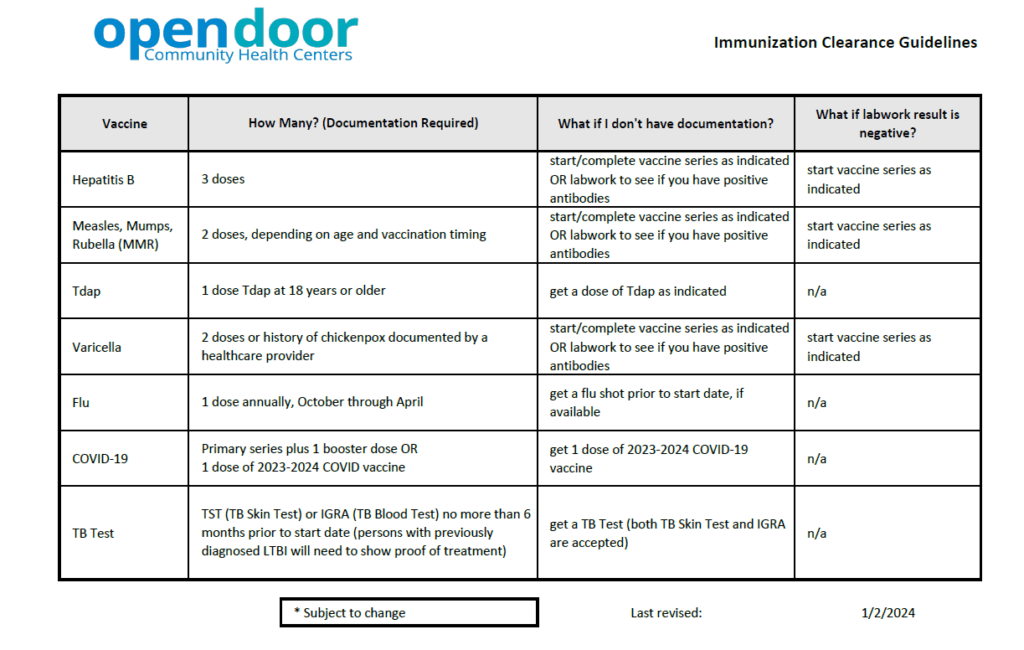
Requirements

Evaluations
Applying
Our APC Residency Program operates on a rolling application basis. Applications are screened continuously, and qualified candidates are invited for interviews as positions become available.
The program begins annually in late August or early September yearly. We encourage applicants to submit their materials early to ensure consideration for the upcoming cohort.
Please access this link to submit your application: https://opendoorhealth.com/np-pa-application-form/
About the Program
We’re training the residents in Open Door’s model of high-performance health care: advanced access scheduling, planned care, the chronic care model, integrated behavioral health and primary care, team-based, with expert use of health information technology and the electronic health record (EPIC).
The residency year begins with intensive orientation to Open Door Community Health Centers, the neighborhoods in which the training sites are located, and the health problems of the target population, and includes walking tours of neighborhoods, tours of Open Door sites statewide, meetings with community leaders, technical training on the electronic health record, and orientation by our chief medical officer to the responsibilities and privileges of medical staff participation at Open Door.
The APC Residency Program has the following goals:
- Increase access to quality primary care for underserved and special populations by training family practice nurse practitioners in a FQHC
- Prepare residents for full and autonomous expert care of complex underserved populations across all life cycles and in multiple settings
- Provide new nurse practitioners (FNPs) and Physician Assistants (PAs) with a depth, breadth, volume, and intensity of clinical training necessary to serve as primary care providers in the complex setting of the country’s FQHCs
- Train new FNPs and PAs in a model of primary care consistent with the Institute of Medicine (IOM) principles of health care and the needs of vulnerable populations
- Improve the clinical skills, confidence, productivity, and job satisfaction of new FNPs and PAs who choose to work in underserved community settings, as well as contribute to their employer satisfaction and workforce retention
- Increase the number of FNPs and PAS ready to serve in leadership roles within community health settings
2024-2026
2023-2024
2022-2023
2021-2022
2020-2021
2019-2020
2018-2019
2017-2018
2016-2017

“The support and continued professional growth offered by the residency program during the often difficult transition from student to provider is priceless. I could not imagine beginning my NP career without it. The organization is welcoming and supportive and the diversity of the patient population provides unique and valuable training opportunities. It has been an outstanding experience I feel lucky to have had the opportunity to be a part of. I wish that all NP’s could have the same supportive start.”
Stephanie Randall, FNP

“I love the fact that when I started Residency and decided to stay on board with Open Door, there was and continues to be support available at all times.There is this constant push for excellence and growth; I love that there are constant ways to hone my craft as I am introduced to up to date treatment guidelines.The patient population and their feedback constantly shows me the reward that comes from giving and the need to continue to be better.”
Values for Residency:
Heal and comfort; serve compassionately
Serve as representatives for Open Doors’ Mission to provide quality care to all people
Foster growth, excellence and positivity
Excel at our craft and find ways to continue to improve. View Self-reflection as a strength
Support and learn from updated research and share with peers; be a lifetime learner
Treat all equally and responsibly use our power for good
Marressa Ozokwere, FNP

Values of Open Door NP Residency:
Promotion of a diverse provider workforce representative of the community it serves.
Dedication to training NP’s to practice at the full extent of their scope.
Promote provider retention in the field of primary care.
Training providers to work in a low resource rural practice setting.
To produce providers that apply their medical knowledge to care for complex medical patients with confidence and compassion.
Testimonial:
“The open door NP residency allowed me to gain confidence taking care of the most complex family medicine patients in a low resource rural practice environment. This program taught me that being a primary care provider is about working as a team at every level to support each other and the patient in achieving their goals of care. The preceptors of this program set the bar for intelligence and compassion, each is dedicated to educating and supporting the next generation of primary care providers”
Angelo Alfano, FNP
Email: [email protected]
Join us for our Virtual Open House sessions!
TBD
Patricia Carter, APC Residency Program Director
[email protected]